FROM DISCOVERY TO DELIVERY
Neuronal exosomes and the evolution of neurodegenerative disease treatment
Dr. Manda Venkata Sasidhar, Founder, Urvogelbio Pvt Ltd.
Dr. Ganji Praveena, Scientist, Urvogelbio Pvt Ltd.
Neuronal exosomes are revolutionising neurodegenerative disease management. They are unlocking new treatment avenues in diagnostics, drug development, and clinical trial management. This work explores innovative, personalised approaches, transforming traditional challenges into opportunities for enhanced neurological care.

The rising challenge of Neurodegenerative diseases (NDDs), including Alzheimer's, Parkinson's, Huntington's disease, multiple sclerosis and others, is mirrored in the growing neurodegenerative drugs market, valued at US$ 36,277.20 million in 2021 and projected to reach US$ 74,809.38 million by 2031. This market, expanding at a CAGR of 7.5 per cent from 2022 to 2031, focuses on conditions that cause progressive neuron damage. Amid this landscape, neuronal exosomes emerge as a significant innovation. These nanoparticles, released by neuronal cells, offer promising cellular communication and drug discovery, development and delivery solutions. By advancing targeted treatments and patient care, neuronal exosomes could play a key role in revolutionising the management of NDDs, aligning with the evolving market trends and medical needs (Huo et al., 2021). The surge in NDDs can be attributed to several interconnected factors:
1. Ageing Population:
NDDs are primarily age-related disorders. As life expectancy continues to increase globally, a more significant proportion of the population is reaching the age where they are more susceptible to these diseases. By 2050, the number of people aged 60 and older will reach 2 billion, nearly double the number in 2020 (Stambler et al., 2018).
2. Genetics and Familial Factors:
Some NDDs have a vital genetic component. The increased understanding and diagnosis of these genetic factors have led to the identification of more cases.
3. Environmental Factors:
Exposure to certain environmental toxins and lifestyle choices, such as poor diet and lack of physical exercise, are increasingly recognised as contributing factors to NDDs. For example, pesticide exposure has been linked to a higher risk of developing Parkinson's disease (Lahiri et al.,2009).
4. Chronic Diseases and Co-Morbidities:
The rise in other chronic conditions, such as obesity, diabetes, and cardiovascular diseases, has a compounding effect on neurodegenerative diseases. These conditions often share common pathways or risk factors that can contribute to the onset or progression of neurodegeneration.
5. Improved Diagnosis and Awareness:
Enhanced awareness and better diagnostic tools have led to more people being diagnosed with neurodegenerative conditions. Previously, many cases may have gone unrecognised or been misdiagnosed, especially in low- and middle-income countries (Lewczul et al.,2018).
6. Globalisation and Urbanisation:
Rapid urbanisation and lifestyle changes are leading to shifts in diet, physical activity, and stress levels, all of which may contribute to the rise in NDDs. Urban areas may also expose individuals to new environmental toxins.
Demographic shifts, genetics, and environmental factors contribute to the rise in NDDS. Thus, improved diagnostics are crucial as they improve disease detection, foster better understanding, and necessitate innovative treatment approaches.
Traditional Challenges in Drug Discovery, Delivery, and Clinical Trials Management
A. DRUG DISCOVERY:
Current Challenges:
• Labour-Intensive Processes: Traditional drug discovery methods rely on highthroughput screening, iterative testing, and manual analysis. The identification of viable targets and subsequent validation consumes significant time and resources (Steinmetz, K. L., & Spack, E. G. 2009).
• Lack of Specificity: Many conventional techniques need more precision to isolate specific biological targets related to NDDs, leading to potential misdirection in research (O'Malley et al.,2019).
• High Costs: The extensive man-hours, specialised equipment, and consumable resources contribute to soaring expenses in the discovery phase.
• Failure Rates: The disconnect between in vitro models and human biology contributes to a high attrition rate, with many compounds failing to progress beyond the early stages (Mullane et al.,2014).
Impact:
• Extended Development Timelines: These challenges result in protracted timelines, slowing the progress of potentially life-saving treatments to the market.
• Frequent Failures: A lack of effective discovery methods contributes to a high failure rate with significant financial implications.
B. DRUG DELIVERY:
Current Challenges:
• Blood-Brain Barrier (BBB): The BBB's function to protect the brain also acts as a formidable obstacle in delivering therapeutic agents to target sites, hindering the treatment of neurological conditions.
• Limited Targeting Capability: Traditional delivery systems often fail to ensure that the drugs reach the specific neurons or regions the disease affects, leading to reduced efficacy.
• Invasive Methods: In some cases, direct injections into the brain or other invasive techniques bypass the BBB, posing significant risks.
Impact:
• Ineffective Therapeutics: Many drugs are rendered unusable for brain-related conditions due to their inability to penetrate the BBB.
• Side Effects and Risks: The necessity to utilise higher doses or invasive techniques can lead to adverse side effects and potential complications.
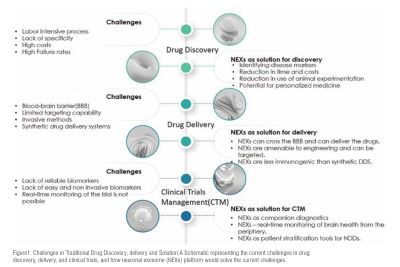
C. CLINICAL TRIALS MANAGEMENT:
Current Challenges:
• Lack of Reliable Biomarkers: Traditional biomarkers often fail to provide an accurate and early assessment of disease progression and response to treatment.
• Invasive Monitoring Techniques: Frequent lumbar punctures or biopsies can be required to monitor treatment, causing patient discomfort and risk.
• Regulatory and Ethical Complexities: The sensitive nature of neurodegenerative conditions introduces additional layers of regulatory and ethical considerations, further complicating trial management.
Impact:
• Prolonged Trials: The challenges above extend trial durations, contributing to the delayed availability of potentially effective treatments.
• Increased Costs: Inefficiencies and imprecisions in trial management inflate costs, burdening research institutions and the healthcare system.
• Uncertainty in Evaluation: A lack of robust monitoring techniques creates uncertainty in evaluating the true efficacy of treatments, potentially leading to erroneous conclusions.
The traditional challenges in drug discovery, delivery, and clinical trial management present substantial obstacles to advancing therapies for NDDs. These problems hinder scientific and medical progress and have profound socioeconomic implications. As the burden of NDDs continues to rise, innovative approaches such as neuronal exosomes offer a promising avenue to overcome these barriers, paving the way for a new era in NDDs research and treatment (Kanojia et al., 2022).
Neuronal Exosome Platform: A Transformative Solution
A. DRUG DISCOVERY:
Neuronal Exosomes as Tools:
• Identifying Disease Markers: Neuronal exosomes encapsulate specific proteins, lipids, and nucleic acids reflective of their cell of origin (brain cells). Analysing these contents allows identifying disease-specific markers and creating targeted drug development opportunities (Schneider, A., & Simons, M. 2013).
• Reduction in Time and Costs: The precise targeting made possible by exosomes can streamline the drug discovery process, reducing the time, labour, and costs associated with traditional methods.
• Potential for Personalised Medicine: Exosome analysis may enable a more personalised approach to drug development, tailoring treatments to an individual's unique genetic and molecular profile.
Neurodex uses exosomes to identify synucleinopathies in dementia using blood-based biomarkers. These vesicles provide minimally invasive, stable diagnostic tools for disease monitoring and progression. Positive data for Alzheimer's diagnosis was shared. Neurodex's innovation promises improved neurodegenerative disease management and therapeutic development.
B. DRUG DELIVERY:
Targeted Delivery:
• Crossing the BBB: Neuronal exosomes can naturally traverse the BBB, offering a targeted and non-invasive method for delivering therapeutic agents to the brain(Younas et al., 2022).
• Enhanced Efficacy and Safety: Encapsulating drugs within exosomes can be directed to specific cellular targets, enhancing treatment efficacy while minimising systemic side effects.
• Versatility in Treatment: Exosome-based delivery systems can be engineered to carry a variety of therapeutic agents, including small molecules, proteins, and RNA-based drugs, expanding the scope of treatable conditions.
Aruna Bio's proprietary neural exosome platform, highlighted by AB126, overcomes the BBB. AB126 (Neural exosome), which are derived from proprietary non-transformed neural stem cells, has a wide range of effects including anti-inflammation, neuroprotection, and regeneration stimulation. This discovery has the potential to revolutionise the treatment of acute neurological conditions and chronic NDDs, with global implications.
C. CLINICAL TRIALS MANAGEMENT:
Real-time Monitoring:
• Non-Invasive Biomarkers: Neuronal exosomes can be isolated from bodily fluids like blood, offering a non-invasive way to monitor disease progression and response to therapy.
• Dynamic Insights: The continuous monitoring made possible by exosomal markers allows for adaptive trial designs, adjusting treatment protocols in real time based on patient response.
• Improved Precision and Reliability: Exosome-based assessments can provide more precise and reliable data, reducing trial duration and costs (Jan et al.,2017).
Multiple sclerosis (MS) is a complex autoimmune disease that affects the central nervous system (CNS) and immune cells. Exosomes, which are essential for cell communication, may shed light on its enigmatic molecular processes. These small vesicles found in bodily fluids carry a variety of contents and have the potential to be used for exosome-based diagnostics in neurologic disorders such as MS.
Neuronal exosomes offer a transformative approach to neurodegenerative disease treatment, addressing challenges in drug discovery, delivery, and clinical trials. This evolving technology paves the way for more efficient and patientcentric methodologies. Collaboration among academia, pharmaceuticals, and biotech firms will be pivotal in leveraging the potential of neuronal exosomes, changing the treatment landscape (Sun et al.,2022). (Figure 1)
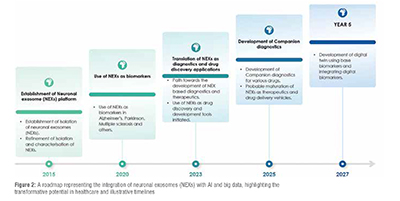
Future Prospects
Integrating neuronal exosomes into drug processes is a promising frontier in personalised medicine, with applications extending beyond NDDs to fields like psychiatry, ageing, and neuroimmunology. Combining exosome research with advanced AI (Figure 2) and big data analytics could enable more refined applications, transforming microscopic insights into actionable knowledge. This burgeoning area represents a potential transformation in understanding, monitoring, and treating diseases, necessitating collaboration and innovation across the scientific community. The future of exosome research holds immense potential, redefining approaches to healthcare and marking a commitment to medical advancement.
Impact of Adoption of Neuronal Exosomes in the Pharma and Biotech Industry
Integrating the neuronal exosome platform offers a transformative approach to the pharmaceutical and biotech industries. By enhancing real-time insights in clinical trials, enabling personalised diagnostics, and streamlining drug discovery, the platform contributes to improved patient outcomes and reduced costs. It also fosters a more ethical approach through non-invasive diagnostics, potentially reducing reliance on animal testing. The overall increase in efficiency accelerates responses to health challenges, positioning the neuronal exosome platform as a critical driver in redefining medical research and intervention, fostering a more effective and compassionate industry.
Conclusion
Neuronal exosomes are revolutionising neurological disorder treatment by enabling innovative drug discovery, targeted delivery, and efficient clinical trials. This technology, validated in practice, heralds a future of patient-centred care with profound industry impact. Investment in neuronal exosomes represents a commitment to more than symptom treatment; it's a stride towards understanding, preventing, and healing at the core of health. This promising step signifies an investment in a future where medicine transcends mere symptom management to embrace holistic healing and prevention.













